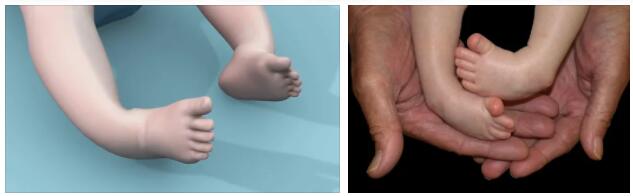
Clubfoot is a congenital malformation of the foot, consisting of pointed, sickle and pes cavus and bowlegs. Clubfoot is clearly visible at birth and should be treated from the start. In most cases, clubfoot can be compensated for with suitable therapy and the children can learn to walk without delay at the right age.
What is clubfoot?
The doctor recognizes a clubfoot at first sight. It is usually a combination of several malformations that can affect just one or both feet. See AbbreviationFinder for abbreviations related to Clubfoot.
Clubfoot is the joint occurrence of pointed, sickle and hollow foot. The foot is turned inwards so that the sole of the foot does not point downwards but towards the other foot.
In addition, the foot is excessively stretched in the ankle and strongly arched in the sole of the foot. Clubfoot is more common in boys than girls and can be unilateral or bilateral. Different strengths are possible. Most children with clubfoot also have strong bowlegs and atrophied calf muscles on the affected leg.
Causes
The causes of the formation of clubfoot have not yet been fully researched. Clubfoot is usually congenital. It is assumed that its origin is genetically determined. The fact that there is a familial cluster strengthens the suspicion of genetic causes.
One theory behind the development of clubfoot is that connective tissue and muscles do not develop in the right proportion during pregnancy and bone growth is impaired. It is also thought to be possible that bone growth stops too early, leaving the feet in the embryonic position and not developing further.
It is also assumed that with genetic predisposition, clubfoot occurs more frequently if the mother smokes during pregnancy. Other circumstances can also promote the occurrence of clubfoot, such as a lack of amniotic fluid or an unfavorable position of the child in the uterus.
Symptoms, Ailments & Signs
The doctor recognizes a clubfoot at first sight. It is usually a combination of several malformations that can affect just one or both feet. If the heel bone is elevated in combination with a steep position in the upper ankle, doctors call it drop foot. If there is a pronounced O-position of the lower ankle, the hindfoot is inclined inwards.
In this case, the heel points inwards. If the toes and metatarsus are turned inwards, there is a sickle foot, while in pes cavus the longitudinal arch of the foot is increased. If there is no treatment, those affected can only walk on the outer edges of their feet. In very severe cases, where the sole of the foot is directed upwards, patients walk on the dorsum of the foot.
While the symptoms in newborns are clear, the doctor carries out further examinations in the unborn child. In this way he ensures that it is actually a case of clubfoot and that the child has not just assumed a clubfoot position. In this context, a shortened, relatively thin calf (the so-called clubfoot calf) is a clear indication that a clubfoot is present. Ultrasound examinations also show clear skin folds that are not present in healthy feet.
Diagnosis & History
The deformity of a clubfoot is clearly visible at birth. With various tests, the doctor can determine whether a real clubfoot is present or whether it is another malposition.
Important criteria are, for example, how much the foot is rotated inwards, how well individual joints are flexible, what is the relationship between foot and calf length, how much the calf muscles have atrophied (wasted away) or whether the blood circulation and sensitivity (the ability to feel) of the leg and foot deviate from the norm.
Complications
If a clubfoot is not treated, the feet will stiffen in the malposition. This results in children walking on the outer edge of the foot instead of on the sole of the foot. An untreated clubfoot affects the whole body and causes further deformities in the hips, spine and shoulders. The clubfoot would stiffen completely over time and cause severe pain.
Early treatment is important for clubfoot. As a result, later complications or worsening of the malposition can be minimized and the symptoms of clubfoot can be treated professionally. Surgical interventions are often necessary to give the clubfoot the best possible functionality. The sooner clubfoot is treated, the sooner good results can be expected.
Complications often occur postoperatively. Clubfoot can suffer permanent damage. Scar tissue formation is a common consequence of surgery. Postoperative bleeding, bruising or injuries to surrounding nerve cords can also occur. As a result, wound healing disorders, a lack of sensitivity or signs of paralysis can occur in the surgical area.
A blood pressure cuff can squeeze nerve cords or vessels. Another complication concerns bone fusion. In the case of clubfoot, the bones may not grow together properly after surgery. This can lead to premature joint wear. The affected joints can become stiff over time. The manufacture of orthopedic shoes is essential for clubfoot patients.
However, this makes a clubfoot much more noticeable. This can lead to psychological stress. Young people with clubfeet in particular often suffer from a lack of recognition, complexes or depression. The development of Sudeck’s syndrome is another possible complication. The bone mass can be progressively degraded. Inflammatory processes in the area around the clubfoot mean severe pain.
When should you go to the doctor?
Optical abnormalities of the foot are an indication of an existing disorder. In the case of a congenital peculiarity of the foot shape, this is already determined at birth by the obstetrician or during the first check-ups of the baby by the pediatrician. In these cases, the newborn’s parents usually do not need to take any action. Further medical examinations and therapy options are automatically initiated by the doctor treating you. In the case of an acquired irregularity of the foot or both feet, a check-up should be initiated independently.
If there are bony malformations, dislocations of the foot or a malposition, a doctor should be consulted. A concern is when forward movement occurs through a rolling motion over the lateral edge or arch of the foot. To prevent further damage to the skeletal system, a doctor should be consulted. If the affected person discovers problems with the muscles in the foot, additional examinations are necessary.
A flexion of the calf muscles or a shortened Achilles tendon are signs of an irregularity that should be diagnosed and treated. Malpositions of the body, a misalignment of the pelvis or pain in the shoulders and neck also indicate existing discrepancies. A visit to the doctor is advisable so that the general well-being is stabilized and the quality of life is improved. If a clubfoot patient develops psychological abnormalities, it is advisable to see a therapist.
Treatment & Therapy
A clubfoot is easy to treat today. It is particularly important to start treatment immediately after the birth and to follow it through consistently. Therapy consists of first placing the foot in the correct position and holding it there. On the one hand, this is done manually, ie a physiotherapist regularly moves the baby’s feet into the normal position.
In addition, a plaster splint is applied, which holds the clubfoot in the desired position. When the child is older, night splints and insoles are used. Ponseti’s clubfoot therapy is particularly well known. The doctor had developed a concept for treating clubfoot with plaster casts and splints within the first four years of life.
If the malposition cannot be corrected with splints, the clubfoot can be corrected with certain operations. It is possible to lengthen the Achilles tendon and thus correct extreme equinus. The position and position of the bones can also be changed surgically.
Outlook & Forecast
Clubfoot is a congenital malformation of the foot. Without the use of medical and medical care, the situation cannot be expected to improve. Spontaneous healing does not occur, nor can the optical conditions be changed by alternative healing methods. Rather, stiffening of the toes or foot is to be expected as the disease progresses. In addition, there are impairments of additional areas of the skeletal system. In addition to pain, those affected often complain about problems in the hips, spine and shoulders. This increases the likelihood of secondary diseases and a further decrease in the quality of life.
When seeking medical treatment, the prognosis depends on the extent of the existing deformity and the cooperation of the patient. In the case of minor impairments, training, special footwear and psychotherapeutic measures are often used. In some cases, medication is given to relieve pain. In most patients, a significant reduction in symptoms can be achieved in the long term through physiotherapeutic support and the independent implementation of special exercises.
In the case of a severe malformation, surgical procedures are used. These are associated with risks, but give the patient the opportunity to achieve lifelong improvement.
Prevention
Since clubfoot is genetic and other causes are not yet known, no preventive measures can be taken. It is important to treat clubfoot immediately after birth and to continue the therapy consistently.
Aftercare
With early and consistent therapy, there are good prospects of recovery. As a result, clubfoot can disappear completely. Since there are no longer any restrictions, no follow-up care is necessary. The patient should only avoid extreme loads. However, this limitation is comparatively marginal.
On the other hand, long-term aftercare becomes necessary if the correction of the clubfoot is not completely successful. In this case, planned examinations are aimed at enabling a normal life despite the limitation. Physiotherapy is an essential element of treatment. They are intended to prevent incorrect posture and to sufficiently stretch muscles and tendons.
The patient must also integrate corresponding exercise units into his everyday life. He is responsible for that. As an aid, the attending physician regularly prescribes orthopedic shoes and insoles. New malformations can only be avoided if they are used consistently. In case of acute problems, the patient turns to the attending physician.
This can detect clear changes in the feet by means of an X-ray image. The follow-up care therefore only affects patients in whom the deformity could not be completely corrected. You need permanent aids to get by in everyday life. Physiotherapeutic exercises are to be carried out at home on your own responsibility. In the case of complications, going to the doctor is inevitable.
You can do that yourself
A clubfoot is a deformity that is congenital or can develop later in life. Affected people can resort to self-help measures that lead to an improvement in the symptoms that occur.
Worsening or further consequential damage can be avoided if an appropriate shoe orthopedist is consulted at an early stage. This malposition can only be counteracted with suitable footwear. However, if individually fitted shoes are not used, those affected must expect a significant deterioration. It is also advisable to see a physiotherapist early on, as this can counteract any circulatory disorders. Regular massage and exercise can promote and improve blood circulation. There are no other measures that you can take yourself and at the same time lead to a significant improvement.
However, regular visits to the doctor are very important and should therefore be strictly adhered to. Regular examinations and explicit exercises can lead to a significant improvement in an existing clubfoot. In addition, possible complications can be avoided, so that a much more pleasant course of the disease can be expected. Own measures are therefore only possible to a limited extent. However, these should by no means be neglected.