When Arachnopathie is a rarely occurring disease, which is associated with the formation of scars in the area of the spinal cord. As a result of these scars, the patients suffer from severe restrictions in their movements and general motor skills. In addition, arachnopathy manifests itself in intense back pain as well as tingling and numbness in the lower extremities.
What is arachnopathy?
As part of arachnopathy, special scars develop in the medulla of the back. This results in considerable impairment of motor skills.
Arachnopathy is a very rare disease of the back. The exact prevalence of arachnopathy has not yet been researched. Although arachnopathy rarely occurs, it has been suggested that a diagnosis is too seldom made.
Instead, many doctors confuse arachnopathy with other back pain conditions, such as a herniated disc . However, arachnopathy requires a fundamentally different therapy.
As part of arachnopathy, special scars develop in the medulla of the back. This results in considerable impairment of the motor skills of people suffering from arachnopathy. In the meantime, various methods of treatment technology have become established that significantly alleviate the patient’s symptoms.
Causes
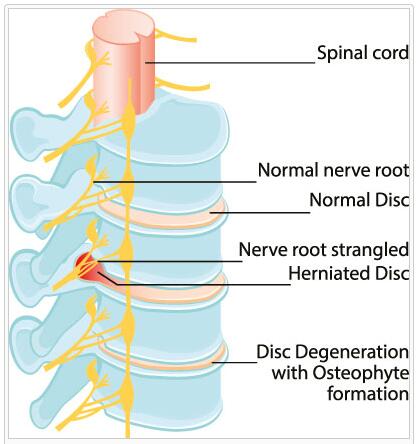
Arachnopathy causes scarring on the medulla of the back. The spine consists of vertebral bodies and intervertebral discs as well as the spinal canal. Inside this canal is the cord of the spinal cord, which runs from the lumbar vertebra along the spine to the skull. The so-called dura mater, a tube with spinal fluid, is located in the spinal cord.
The liquor supports the gliding of the vertebrae. In addition, the spider’s web is located in the dura mater, which is called the arachnoid in medical terms. When congestion forms in the fluid in the spinal cord, increased pressure develops. As soon as this pressure is too great, the liquor evades next to the spine.
This gives the appearance of a spider web. As a result, the affected areas become inflamed and arachnopathy develops. The inflammatory processes result in scar formation on the spinal cord. This results in enormous pain and restrictions in mobility .
Symptoms, ailments & signs
The signs of arachnopathy are often misleading to confuse the disease with other diseases of the back. Because the main symptom is usually extremely severe pain, which is also possible with herniated discs. The pain of arachnopathy is mainly localized in the lower part of the spine.
In addition, the pain sensation in arachnopathy often extends to the lower limbs or the entire body. In addition, patients with arachnopathy feel a tingling sensation in their legs . Also, numbness and weakness attacks are possible. Sometimes the muscles cramp and the functioning of the bladder and intestines are impaired. Chronic pain that restricts motor skills is characteristic of arachnopathy.
Diagnosis & course
The diagnosis of arachnopathy is usually made by an orthopedic surgeon . A thorough medical history with the patient is particularly important in order to reduce the risk of confusion with herniated discs. However, misdiagnoses are still common because the symptoms are very similar and the arachnopathy is less common and therefore less well known.
The patient reports on his or her medical history, the onset of the pain and possible development factors. He also informs the doctor about possible diseases of the back and spine in the past. The clinical examinations initially consist of tests of the patient’s mobility.
The specialist then uses imaging techniques to reduce the risk of misdiagnosis and to identify the exact location of the scars on the spinal cord. The doctor usually performs an MRI scan and takes layer-by-layer images of the spinal cord. In this way, the locations of the scar formation can be detected and confusion with herniated discs is greatly reduced.
A corresponding differential diagnosis is necessary in every case. It is also possible that the arachnopathy occurs at the same time as a herniated disc and that suitable therapeutic measures for both diseases are required.
Complications
Arachnopathy can cause a number of complications. First of all, the disease is accompanied by chronic and persistent pain in the lower back area, which in some cases can radiate into the legs or even the entire body. The typical symptoms such as tingling or numbness sometimes develop into muscle cramps and a pronounced feeling of weakness in the arms and legs.
Sometimes disorders in the bladder and intestinal area also occur, which make urination and bowel movements difficult and, if the course is chronic , can lead to incontinence . If the course is severe, there will also be impaired motor skills and sensory disorders in the affected limbs. The complications, which can be severe at times, mostly only occur in the later course of an arachnopathy.
However, the unspecific general symptoms often lead to misdiagnosis by those affected. Accordingly, the disease is often diagnosed late; usually only when the complications mentioned are already fully developed. With early treatment, the risks are limited to possible allergies to prescribed drugs and possible surgical incidents. The complications usually also disappear after a successful procedure.
When should you go to the doctor?
If inexplicable pain persists in the lower spine, a doctor should be consulted. Through an examination, the doctor can find out whether the symptoms are due to arachnopathy or some other disease. If the problem is arachnopathy, further therapeutic measures are required. Medical diagnosis and treatment are necessary at the latest when further symptoms occur. Warning signs of arachnopathy can also include feelings of numbness and weakness, and a tingling sensation in the legs.
Muscle cramps and dysfunction of the bladder and intestines are also rare. However, it is characterized by chronic pain, which increasingly restricts motor skills as the disease progresses. If one or more of these symptoms occur, it is essential to consult a doctor about the symptoms. Sensory disturbances and incontinence suggest that the arachnopathy is already advanced. A visit to the doctor should then no longer be postponed. Even in the late stages, the disease can usually be treated well with a successful intervention.
Treatment & Therapy
Arachnopathy can now be treated relatively well. The treatment usually takes place in a specialized clinic using thecaloscopy. This form of therapy is a minimally invasive method, whereby a small incision in the diseased area serves as an entrance for a movable endoscope.
The instrument examines the affected area and takes targeted action against the scars. In the majority of cases, patients no longer feel any pain after a successful procedure. Restrictions of movement and sensory discomfort also disappear.
Outlook & forecast
With medical treatment and the cooperation of the patient, the chances of recovery from arachnopathy can be classified as good. Without medical care, the person affected can initiate various possibilities and training courses for self-healing, but will only experience complete freedom from symptoms in a very unlikely case. Nevertheless, it is advisable to use the self-help methods independently. These help prevent relapses and alleviate existing symptoms.
With medical therapy, the likelihood of a cure increases immensely. The forecast outlook has been significantly improved in recent years with the scientifically proven methods given. The necessary corrections are made in a surgical procedure. This is done routinely and is completed within a few hours. The patient is usually discharged after a few days of inpatient stay. Then, in a healing and rehabilitation process lasting several months, the disease is cured and the symptoms subside.
It must be taken into account that this process depends on the patient’s previous illnesses or other existing complaints. Mid-adult people with no disease have a good chance of a cure. However, relapse symptoms can occur at any time. For this reason, the methods learned in aftercare should continue to be used to improve movement sequences or posture.
Prevention
So far, no reliable statements can be made about effective preventive measures in relation to arachnopathy. The mechanism of the pathogenesis of arachnopathy is partly known and researched, but the exact causes are partly still unclear. It has been suggested that there are various external risk factors that cannot be avoided in every case.
For example, physically strenuous work and lifting heavy objects are influences that may have a beneficial effect on the development of arachnopathy. However, arachnopathy is still a rare disease. With a quick diagnosis and the successful use of modern therapeutic methods, arachnopathy can usually be treated well, so that most of the affected people live again without pain in the back and with full mobility.
Aftercare
Because arachnopathy can relapse after successful treatment, follow-up care is very important. In this case, it offers the opportunity to avoid relapses and alleviate any remaining symptoms. Since the medical treatment of arachnopathy is an invasive procedure, it is important to pay particular attention to personal hygiene after this procedure.
This can reduce the risk of ignition. In addition, it can be helpful to care for the affected areas with special care products to ensure a better healing process for the wound. Since it can take some time after the procedure for symptoms to subside, there are measures that can help improve your quality of life.
This includes, for example, gymnastics or sports such as swimming. These measures are very well suited to counteract muscle spasms or to alleviate any discomfort in the extremities. If numbness occurs with arachnopathy, acupuncture can help during follow-up until the symptoms are relieved by treatment.
If the bladder and bowel function is impaired, attention should be paid to an appropriately balanced diet during aftercare. A diet with sufficient vitamins and fiber and a healthy lifestyle with enough exercise promote regulation of the bladder and intestines.
You can do that yourself
Arachnopathy can make everyday life much more difficult for those affected. Various measures and tips make life easier with the disease and its consequences.
First of all, preventive measures are recommended. Once diagnosed, symptoms such as paralysis and incontinence can be treated symptomatically using aids such as a wheelchair or adult diapers. The causal disease should be treated as soon as possible. Suitable specialists can be identified by talking to the family doctor or through information brochures and forums.
After treatment, those affected should ensure adequate personal hygiene . The affected areas of the skin are best treated with suitable care products from the pharmacy . As an alternative, there are ointments and applications from nature. Aloe vera , garlic oil and apple cider vinegar have proven effective . The use of natural remedies should always be done in consultation with the doctor.
Sports measures such as gymnastics or swimming help against abnormal sensations and muscle cramps. The numbness can be counteracted by massages or acupuncture . In addition, dietary measures are recommended. A balanced diet rich in fiber regulates the activity of the bladder and intestines, which are often disturbed in arachnopathy.